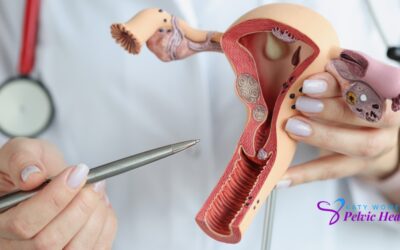
There’s no need to suffer in silence if anyone has a pelvic or bladder problem. The urogynaecology group’s doctors offer thorough and compassionate care that is customized to each patient’s condition. The treatment approach will be determined by the nature and source of the issues the patient is experiencing.
What Is a Urogynecologist and What Do They Do?
Urogynecologists deal with problems involving the pelvic muscles and bladder. Overactive bladders, weakened pelvic muscles, sexual difficulties, and bladder or rectal incontinence are all examples of this. Patients are evaluated, diagnosed, and treated. They’ve been specially trained to assist ladies in situations like these:
- Incontinence due to stress
- Urge incontinence
- UTI’s
- Bladder leakage
- Bladder pain
- Other circumstances
Understanding Urogynaecology
Urogynaecology is a subspecialty of obstetrics and gynecology that focuses on female pelvic care and reconstructive surgery. Nearly all urogynaecological disorders can be recognized and treated successfully with moderate lifestyle modifications, drugs, or surgery. The optimum treatment for each patient may differ due to a variety of characteristics that are unique to each person. The patient’s age, amount of physical activity, previous treatments and medications, sexual activity, and, eventually, the patient’s aspirations are all aspects that can influence whether treatment is preferred.
Treatments for urogynaecology that do not require surgery
Once a urogynecologist problem has been identified, the urogynecologist will discuss all options for treatment with the patient. Because many nonsurgical alternatives are straightforward and have few, if any, adverse effects or dangers, they are frequently the first choice considered. The following are some of the non-surgical treatments that our advanced urogynaecology specialists do in-office:
Cystoscopy, which enables specialists to see inside the bladder
Urodynamic testing enables clinicians to see how the bladder responds when it is pumped and drained.
Vaginal pessary, which is a silicone therapy equipment designed to address prolapse and incontinence without operations.
Posterior tibial nerve stimulation is used to address the nerves that control bladder and pelvic floor function.
Kegel exercises, commonly known as pelvic floor muscle training exercises, are a type of pelvic floor muscle strengthening exercise.
Injections to help with bladder control issues
Additional operations are also carried out in the office. These are some of the most prevalent treatment options for patients who don’t want to have surgery but yet want to solve their bladder problems. The urogynecologist will inquire about the symptoms, their timing, and their impact on quality of life throughout the consultation. They will also go through the patient’s medical history as well as any previous occurrences that may have had an impact on the pelvic floor.
What Kinds of Surgical Procedures Does Urogynecologists Do?
At Katy Women’s Pelvic Health, we strive to deliver the simplest, least intrusive therapies for pelvic discomfort and urogynaecology problems. Surgery is often the only or most effective choice for certain disorders, such as pelvic organ prolapse or urine incontinence. The physician collaborates with a treatment team that comprises a nurse practitioner, a medical assistant, and a physical therapist. If surgery is recommended by the specialist, it could include any of the following:
- Restoring pelvic floor function
- Taking care of any prolapse
- The uterus could be removed (hysterectomy)
- Mesh mid-urethral sling for urinary leaking
- Anal or sphincter muscle repair
In addition, procedures such as robotic hysterectomies are sometimes available in-office for patients who are interested. These operations are frequently significantly more intrusive than many of the procedures performed by one of our advanced urogynaecology experts, and they can take a long time to recover from.
Who Is a Good Surgical Candidate?
A number of criteria go into determining whether or not someone is a good candidate for urogynaecology operations. If both the patient and the doctor agree that surgery is the best option, patients must meet a number of prerequisites before surgery can take place. Patients must, above all, be in generally good health. Finally, patients must be free of any major underlying health issues that could interfere with the anesthetic or result in excessive blood loss. Patients must also not be sick at the time of surgery, as this increases the risk of infection and slows the healing process.