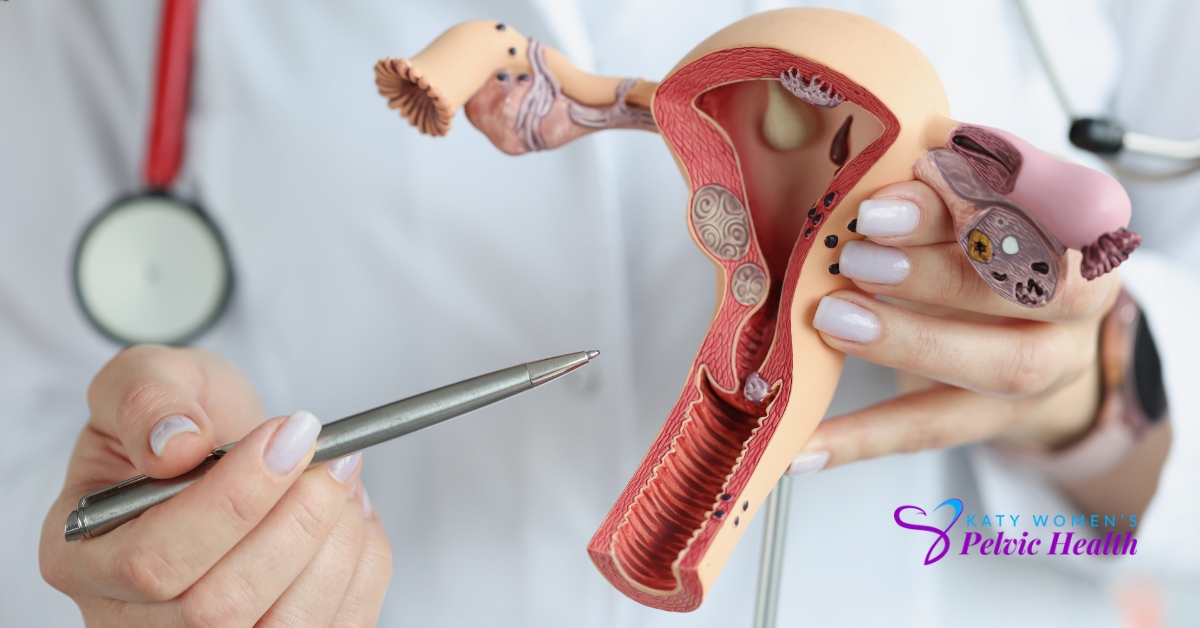
Urogynecology, a surgical subspecialty of gynecology and urology, specializes in treating problems with the female pelvic floor.
The American Urogynecologic Society states that “the pelvic floor is a set of muscles, ligaments and connective tissue in the lowest part of the pelvis that provides support for a woman’s internal organs, including the bowel, bladder, uterus, vagina and rectum.”
Among the problems of the female pelvic floor are fecal incontinence, organ prolapse, stress urinary incontinence, and overactive bladder.
After graduating from medical school, a physician must complete a residency in either obstetrics and gynecology OR urology before becoming a urogynecologist. The doctor will next undergo additional training and certification in reconstructive surgery and female pelvic medicine. These fellowship programs, which normally run two to three years, give the doctor extra knowledge.
Table of content
● Problems related to Urogynecology.
● Signs and Symptoms
● Seeking doctor
What are the Problems related to Urogynecology?
Urogynecology problems like incontinence or discomfort during sex may be greatly reduced or eliminated with therapy. To help you get back to living life to the fullest, you and your medical team will collaborate to identify the optimum therapy or treatment combination.
Non-operative therapies
● Injections for urine leakage and incontinence: Bulking substances can be used to treat stress incontinence. Urge incontinence or overactive bladder can be treated with injections of the Botulinum toxin. Both procedures can be performed in-office or as an outpatient by using a local anesthetic.
● Medications: Medication may be used to treat some illnesses and incontinence problems.
● Nervous system stimulation: Nerve stimulation similar to acupuncture may be used to treat overactive bladder.
● Kegel exercises, commonly referred to as prolapse exercises, which strengthen the pelvic floor muscles, may help with some of the symptoms of the illness. In these exercises, the pelvic muscles are contracted and relaxed. They are unable to fix more severe prolapses, even if they might help with some symptoms.
Treatment that Needs Surgery
Procedures for Prolapse
These techniques strengthen the pelvic floor while repairing the prolapse. There are numerous treatments available for prolapsed organs. The options include
● construction of a new vagina
● Small intestinal or rectal support
● The support of the sphincter
● Uterus-removing surgery
● an operation to regain bladder control
Having incontinence surgery
Surgery might be a viable approach to treat incontinence brought on by bladder pressure.
● Techniques for slings: A hammock or possibly your muscle supports the urethra.
● An artificial bladder pacemaker: An implanted device may be used to treat urine incontinence and overactive bladder.
Prolapse
Pelvic organ prolapse is a disorder when one or more pelvic organs slide into the vagina. The uterus, colon, bladder, or vaginal apex are all potential suspects. Do not become alarmed if an incontinence prolapse is causing you pain and suffering. Usually, strengthening the pelvic floor muscles and making lifestyle changes are enough to reduce symptoms, but occasionally, medical intervention is necessary.
Urinary Incontinence
Urinary incontinence, or the inability to control one’s urine, affects many people. The degree of urgency might range from the infrequent leakage of urine when you sneeze or cough to the sudden, intense urge to urinate that causes you to miss the bathroom.
Although urinary incontinence is becoming more prevalent as people age, it is not a given. If your daily activities are being affected by urine incontinence, speak with your doctor. The majority of the time, the symptoms of urinary incontinence can be addressed with simple dietary and activity modifications or by seeing a doctor.
Pelvic Augmentation
Pelvic organ prolapse is the term used to describe the prolapse of the pelvic organs when the pelvic floor tissues are torn or destroyed, which happens frequently after delivery. Surgery, extended illness, or recurrent heavy lifting could possibly be to fault. A procedure called pelvic reconstruction uses many techniques to fix the prolapse.
What Signs Might a Woman Have That a Urogynecologist Should Examine?
Women often feel uncomfortable discussing their pelvic floor issues with their doctors because of the symptoms they encounter. In this situation, it makes sense to consult with a professional who has received specialized training to assist with these feminine concerns.
It’s possible for symptoms to appear gradually and worsen over time. Women may encounter the following signs:
● a problem entirely emptying the bladder or urinating
● When you laugh, exercise, or cough, urine leaks.
● Need to urinate immediately
● Urinary tract infections frequently
● A lump on the genital wall
● pulling or discomfort in the cervix
Frequently, these symptoms will get worse at night or right after a bowel movement.
A Pelvic Floor Disorder: What Is It?
The bladder, uterus, vagina, and rectum are all supported by the pelvic floor in women. It is supported by the nearby muscles, ligaments, connective tissues, and nerves. These tissues and muscles support the body parts in carrying out their specific functions.
The structures that hold various body components in place are frequently referred to as the sling or hammock. The bladder, uterus, vagina, and rectum are all affected by the bladder, uterus, vagina, and rectum when these supports are damaged or compromised. The fundamental problem with the pelvic floor is this.
Fecal incontinence, urine incontinence, or prolapse of the pelvic organs are the three most prevalent pelvic floor disorders.
What Leads to a Prolapse and Why?
One of the varieties of pelvic prolapse can occur for a number of different reasons.
A woman who vaginally delivers a baby may have prolapse issues. Births by C-section can also result in a prolapse. Multiple pregnancies increase a woman’s likelihood of developing this illness.
Smoking, genetics, and other factors can all affect the problem. It could be troublesome if a lady experiences persistent constipation or a persistent cough.
The age of the person is one of the main causes. Women who are past childbearing age frequently have a higher risk of pelvic floor rips or weakness.
When to See a Doctor
If you encounter any of the above-mentioned diseases or symptoms, as well as other symptoms like:
● An obvious protrusion or bulging in the vagina
● Feelings of fullness, heaviness, tugging, or pain in the vagina, particularly at night or when passing stool
● Having trouble urinating or completely emptying your bladder
● when you cough, laugh, or move quickly causes incontinence
● frequent and urgent urination needs
● having frequent urinary tract infections
Reference
https://www.petermlotzemd.com/urogynecology-7-fast-facts/
https://www.greaterbostonurology.com/blog/gbu-blog/2017/07/what-is-urogynecology